Do you have HIV? Do you inject drugs?
If you answered yes, this resource is for you. Keep reading!
This resource has information on HIV treatment for people who inject drugs and have HIV. It also has information on how to take care of yourself and keep others safe.
What is HIV?
HIV is a virus that is usually passed through sex or from sharing equipment (works) for injecting drugs. HIV can make it difficult for your body to fight infections.
HIV can make you very sick if you do not get the care you need. With proper treatment and care, people living with HIV can live long and healthy lives and avoid passing HIV to others.
Finding out you have HIV can be difficult.
Give yourself some time to take in the news.
Talking to a friend or family member may help.
Lots of people can stay healthy and live for a long time with HIV.
When you are ready, here are some things you can do:
- Talk to a nurse or health worker.
- Talk to other people who are living with HIV.
- Ask your doctor about treatment for HIV.
HIV treatment can help you
The sooner you start treatment for your HIV, the better your chances of staying healthy (or getting healthy again if HIV has made you sick).
For many people, treatment means taking one pill once a day.
Treatment cannot cure HIV, and it is a life-long commitment. But it can help you stay healthy for a long time.
If you use drugs you can still get treatment for HIV.
You deserve respectful care by doctors, nurses and other health workers. You can ask harm reduction workers or other people who use drugs about which doctors and nurses are good to work with.
HIV treatment helps prevent passing HIV
Taking HIV treatment also helps prevent passing HIV to others. HIV treatment lowers the amount of HIV in your body. Treatment can lower the amount of HIV in your body to a level so low that tests can’t detect it. This is called having an undetectable viral load.
If you maintain an undetectable viral load you will not pass HIV through sex, and the chance of passing HIV from sharing needles is dramatically reduced.
Treatment is more than just taking medicine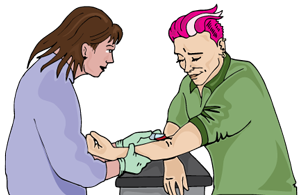
Besides taking medicine, HIV treatment involves seeing a doctor regularly. Most people with HIV need to see a doctor every six months.
At these appointments, a doctor will do blood tests to check if your HIV medicine is working.
If your medicine is not working, the doctor might change your medicine. If you are having problems remembering to take your medicine or if you have side effects, you can ask a doctor or nurse for help.
Need help but not sure who to ask?
Talk to a nurse, doctor or support worker who knows about treatment.
They can help you.
Having problems with your treatment?
Getting treated for HIV means that you have to take medicine as prescribed.
Remembering to take your medicine regularly can be difficult. But if you forget to take your medicine, your treatment may not work and you may need to switch medicine.
HIV treatment is a lot easier to take than it used to be. Many people do not have side effects at all, but you may have side effects with your treatment. These side effects often go away or get easier to handle after you have been on treatment for a while.



 If you are having problems with your treatment, talk to your health worker. They can help you.
If you are having problems with your treatment, talk to your health worker. They can help you.
Using street drugs and taking treatment
If you are being treated for HIV and you use drugs, be as honest as you can with your pharmacist and doctor about all the street drugs and medicines you are taking. Some kinds of HIV medicine can change the effects of street drugs, so your doctor might avoid prescribing certain HIV medicines.
HIV medicine can also change the effects of methadone and buprenorphine. If you take methadone or buprenorphine, your doctor might change the dose when you start taking HIV treatment.
Taking street drugs can make it hard to remember to pick up prescriptions and take your HIV medicine as prescribed. Talk to a health worker about any challenges you are having. They can
help you.
Getting treatment in prison
If you are at risk of being arrested or going to prison, you may want to keep your doctor’s phone or fax number on you.
If you are being treated for HIV, you have the right to keep getting treatment in prison. Your treatment should not be stopped when you go to prison.
You may want to memorize the names of all your medicines. Then you will be able to tell the prison’s health workers which medicines you take.
If you have questions or need support for HIV treatment in prison, you can call PASAN. PASAN is a group that supports prisoners living with HIV and/or hepatitis C. You can call PASAN toll-free at 1-866-224-9978. If you aren’t able to call the toll-free line, you can call PASAN collect at 416-920-9567.
Taking care of yourself and keeping others safe
Taking HIV treatment is one of the best things that you can do to keep yourself healthy and help to prevent passing HIV to other people.
The rest of this resource talks about other things you can do to take care of yourself and keep others safe.
Things you can do to stay healthy
Having HIV can be hard on your body, but you can do many things to stay healthy. You can:
 Drink water.
Drink water.- Try to get enough sleep.
- Eat as well as you can.
- Talk to someone about how you are feeling.
Using drugs, smoking cigarettes and drinking alcohol are also hard on your body. Some people decide to change their use after they find out they have HIV. Talk to a nurse or a health worker if you want to make a change. They can help you.
How HIV can pass from person to person
HIV is in the blood.
HIV can pass from one person to another when people share works when injecting drugs.
HIV can also pass from one person to another when somebody gets a piercing or a tattoo if the artist does not sterilize the tools or the artist re-uses ink.
HIV is in cum, pre-cum, vaginal fluid or pussy juice, and anal fluid or bum juice. This means that HIV can pass from one person to another during sex (if the person with HIV is not on successful treatment).
HIV is not in spit, sweat or tears. It cannot be passed by things like handshakes, kisses, coughs, swimming pools, toilet seats, towels, forks, cups, food or animals.
Hepatitis C can also be passed through sharing works
You can get hepatitis C from sharing works, including needles, syringes, filters, washes, water and cookers. You can also get it from using another person’s pipe, stem, mouthpiece, rolled paper or straw for smoking and snorting drugs.
Hepatitis C is a virus that injures the liver. There are other types of hepatitis, including hepatitis A and B. You can also get hepatitis B from sharing works.
There are vaccines for hepatitis A and B. Talk to a health worker about getting these vaccines.
There is no vaccine for hepatitis C but treatment cures over 95% of people with hepatitis C. You don’t need to stop using drugs to get hepatitis C treatment.
The only way to know for sure if you have hepatitis C is to get tested. Go to the section on getting tested regularly for information about testing.
Taking care while injecting drugs
If you inject drugs, try not to borrow or lend any works for injecting drugs.
The blood on the works could be too small to see.
If you use all new works all the time, there is NO chance of passing on HIV or getting hepatitis C while injecting drugs.
Here are two other good reasons to use new works:
- New needles are sharp and less likely to hurt your veins.
- Using new works helps make sure you do not get sick from blood clots, cotton fever and other infections.
All these things should be new:
| Needle |  |
| Cooker |  |
| Filters |  |
| Vitamin C powder or citric acid |  |
| Sterile water |  |
| Alcohol swabs |  |
| Your tie (tourniquet) does not need to be new every time if you are the only one using it. Get a new tie if you see any blood or dirt on your tie. |  |
Being in control of when and how you get high
If you need someone else to get you high, you may go into withdrawal because you cannot get high when you need to.
Try to take control over how and when you get high.
To have more control over your drug use:
- Learn how to inject yourself. If there is a street nurse in your community, they can show you how.
- Know your dealer so you can buy your own drugs if you need to.
- Try to use with people you trust and in a place where you don’t feel rushed.
If someone is having an overdose
Opiate overdoses are the most common. Opioids are depressants that slow the body down, especially our breathing. They include fentanyl, carfentanyl, heroin, oxycodone and others. If someone won’t wake up or is having a hard time breathing, they might be having an opiate overdose.
Stimulants can also cause an overdose. Stimulants or “uppers” like amphetamines, crystal meth, cocaine and MDMA (Ecstasy or Molly) speed the body up. If someone is having crushing chest pain or seizures, or if they are unconscious or in-and-out, they might be having a stimulant overdose.
If you think someone is having an overdose, call 911. Stay and help. Even if you’ve taken drugs or have some on you, the Good Samaritan Drug Overdose Act can protect you from being arrested.
Use naloxone, if you have it. Naloxone reverses an opiate overdose and can save someone’s life. Naloxone will not reverse a stimulant overdose but it can still help if a person has taken a mix of drugs. When in doubt, use naloxone. It’s safe.
If naloxone is available where you live and you want to learn how to use it talk to a harm reduction worker about how to get training.
Tips to prevent an overdose
Avoid using alone. Use with someone you trust or at an overdose prevention site, if there is one in your community. These are places for people to use drugs with a health worker on site. The health workers can help if there is an overdose and provide tips for safer use.
Start low, go slow. Test a small amount first. Drugs may be more potent than you realize, especially if you’re buying from a new dealer.
Avoid mixing substances. This can contribute to an overdose.
Take care of yourself. Use less when you’re having health issues or if you haven’t used for a while, for example if you’ve recently been released from prison or the hospital or if you’re returning from travel.
Have an overdose plan. Carry naloxone, know how to use it and let others know you have it. Make sure someone can call 911.
HIV treatment is very safe, but some types of HIV medicine can change the effects of the street drugs that you use. This could contribute to an overdose. Talk to your doctor about whether the HIV medicine you take could change the effects of street drugs.
Being safe when getting a tattoo or piercing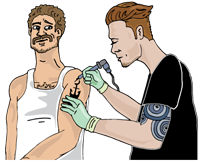
The same infections that can be passed from sharing works can also be passed from getting a tattoo or piercing with equipment that is not new or properly cleaned.
Whether you are getting a tattoo or piercing at a professional studio, at home or in prison, it’s safest when the artist uses:
- A sterile tattoo machine or piercing equipment.
- New needles.
- New ink.
- New ink pots.
- New latex or vinyl gloves.
If the artist works in a professional studio, make sure they use a special machine called an autoclave, which sterilizes equipment.
Infections that can be passed though sex
Some infections can be passed through sex. They are called sexually transmitted infections (STIs). Some of the most common STIs are HPV, chlamydia, gonorrhoea and herpes. Syphilis is less common. In rare cases hepatitis C can be passed through sex.
The only way to know for sure if you have an STI is to get tested. Go to the section on getting tested regularly for information about testing.
Staying safe and protecting your partners when you have sex
HIV and STIs can pass from person to person during sex.
There are lots of ways to be safer when you have sex.
Use the ways that are best for you.
- Keep some condoms and lube around to use when you have sex. Condoms help to prevent HIV and STIs.
- Taking your HIV medicine helps prevent passing HIV. If you are on treatment and maintaining an undetectable viral load you will not pass HIV through sex.
- If you have a sex partner who does not have HIV, they can think about taking a medicine called PrEP (pre-exposure prophylaxis) that helps prevent HIV.
- There is little to no chance of passing HIV to a partner from oral sex (blow jobs or pussy eating).
Preventing passing HIV to a baby
HIV can pass to a baby during pregnancy, birth and breastfeeding (chestfeeding).
The good news is that with care and treatment, you can have an HIV-negative baby.
If you have HIV and are thinking about having a baby, talk to a nurse or doctor.
If you have HIV and think you are pregnant, talk to a nurse or doctor.
 Getting tested regularly
Getting tested regularly
It’s a good idea to get tested regularly for hepatitis C and STIs. If you have not been vaccinated against hepatitis A and B you should also get tested for them.
A nurse or doctor can give you these tests. They can also tell you how often to get tested.
To find out where to get tested, ask a health worker or go to www.hiv411.ca.
If you find out that you have an infection, talk to your nurse or doctor about your treatment options.
Tips for getting a blood test if you have bad veins
The tests for hepatitis A, B and C and some STIs are blood tests. Getting blood tests can be difficult if you have bad veins, but there are things you can do to make the test easier:
- Show the nurse or doctor your best veins.
- Warm your body by taking a shower just before you go for your blood test and wear warm clothes to your test.
- Drink two or three glasses of water one to two hours before your test.
- Bring a friend for support.
- Talk to your nurse or doctor about other ways to make blood tests easier.
Where can you get more information about HIV?
For information about HIV:
- Talk to a doctor or nurse.
- Get in touch with a support worker at your local HIV organization.
Production of this document has been made possible through a financial contribution from the Public Health Agency of Canada. The views expressed herein do not necessarily represent the views of the Public Health Agency of Canada.
CATIE thanks all of the community and medical reviewers who contributed their expertise to previous versions of this resource. We also thank BCCDC Harm Reduction Services
@ towardtheheart.com for providing content related to overdose for this version.

