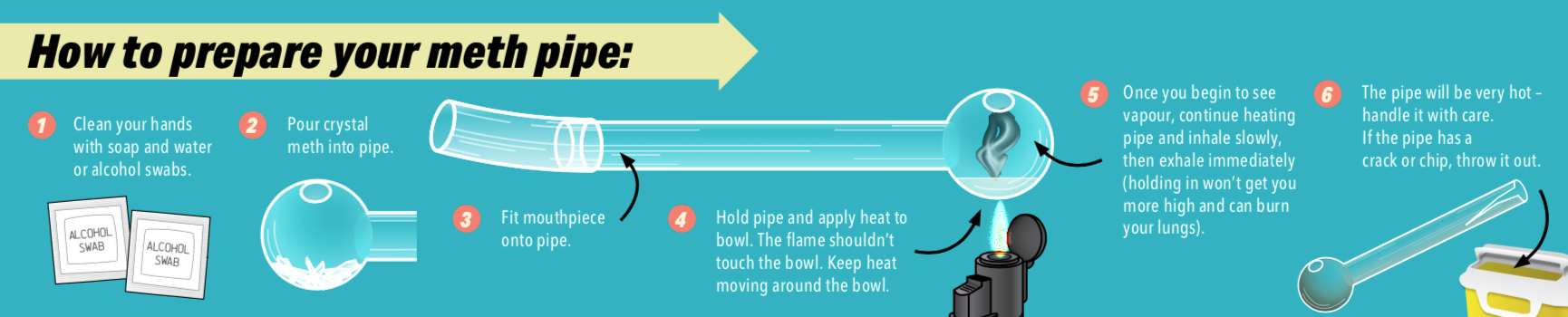
How to prepare your meth pipe
- Clean your hands with soap and water or alcohol swabs.
- Pour crystal meth into pipe.
- Fit mouthpiece onto pipe.
- Hold pipe and apply heat to bowl. The flame shouldn’t touch the bowl. Keep heat moving around the bowl.
- Once you begin to see vapour, continue heating pipe and inhale slowly, then exhale immediately (holding in won’t get you more high and can burn your lungs).
- The pipe will be very hot – handle it with care. If the pipe has a crack or chip, throw it out.
Supplies you use to smoke crystal meth safer
- Bowl pipe
- Mouthpiece
- Alcohol swab
- Torch lighter
This resource provides information about how to smoke crystal meth with this equipment. Talk to your local harm reduction site about which safer drug use supplies are available and how they are meant to be used.
Safer crystal meth smoking tips
- Avoid using alone.
Try to smoke in a safe place with people you trust. - Start low, go slow.
The crystal meth may be more potent than you realize. - Know the source of your drugs.
Try to prepare doses yourself. - Avoid mixing substances.
Mixing with opioids can lead to a fatal overdose. - Have condoms and lube with you.
You may want to have sex while high. - Connect with others.
Ask them to reach out to make sure you’re okay. - Take care of yourself.
Try to eat something before you smoke. Stay hydrated with water or juice. - Be kind to yourself and your skin.
Wash your hands after smoking. - Take a break.
Get some sleep, drink water or juice and eat something.
Combining substances can be dangerous
- Erectile drugs (Viagra, Cialis) put extra strain on the heart, cause sudden shifts in blood pressure and can lead to stroke, chest pain and heart attack.
- Other stimulants, like MDMA or cocaine, can push your body too far, increasing the risk of overheating or stroke.
- Downer drugs, like GHB, can lead to stroke or heart attack.
- Alcohol & stimulant drugs (MDMA, cocaine) can dehydrate the body further when mixed. This can negatively affect kidney and liver function and make crash symptoms worse.
Mouth care
- Drink water or juice to keep your mouth moist and reduce cracks and blisters.
- Moisten your lips with your own lip balm.
- Chew gum to keep your mouth moist and reduce clenching.
- Brush your teeth when possible or use mouthwash.
- Avoid infection by using your own mouthpiece or pipe and not sharing it.
Use your own stem and mouthpiece to prevent hepatitis C
Hepatitis C can be passed through tiny amounts of blood on meth smoking equipment. Talk to a harm reduction worker about where to get equipment and where to get tested for hepatitis C.
Smoking meth can lead to skin issues such as infections, lesions or abscesses that may require medical attention.
Stimulant overamping and overdose
Fatal overdoses are not common with stimulant use, however the drug supply is unpredictable and a fatal overdose is possible. Overamping can be considered a type of non-fatal overdose. This information is to help identify when a person is overamping and needs to rest, and when a person goes down and needs emergency medical services.
Overamping |
Overdose (OD) |
|---|---|
| Signs of overamping
Effects of the high can become more extreme with meth over-use. This happens more often when someone hasn’t slept or eaten in a while. These can include:
|
Signs of a stimulant overdose (OD)
|
If you have to leave the person alone, put them in the
RECOVERY POSITION

Naloxone reverses an opioid overdose. There is no antidote to stimulant overdose, but the drug supply is toxic and unpredictable. Giving someone naloxone will not harm them. When in doubt, use naloxone. IT’S SAFE. Talk to your harm reduction worker about where to get support and help if you want to reduce or stop your crystal meth use.
Thank you to the Ontario Harm Reduction Distribution Program (OHRDP); Jennifer Broad and Keith Williams from the Toronto Community Hepatitis C Program; Natalie Kaminski from the Peel Region Drug User Network; Toward the Heart BCCDC Harm Reduction Services; Street Works; Nine Circles; and HANDUP for their help in the development of the resource.
Design and layout: Pam Sloan Designs.
CATIE project leads: Rivka Kushner and Melisa Dickie.
This resource is adapted from a brochure by the Ontario Harm Reduction Distribution Program (OHRDP), 2014, which adapted an original resource by Vancouver Coastal Health, 2011.
Production of this publication has been made possible in part through financial contributions from the Ontario Ministry of Health and the Public Health Agency of Canada (PHAC).
The views expressed herein do not necessarily represent the views of our funders.